Persistent power outages in Nigeria do more than inconvenience households and disrupt businesses; they also silently determine who lives and who dies. Nowhere is this reality more brutal than in neonatal intensive care units, where the smallest patients depend entirely on electricity to survive. IBRAHIM ADAM reports that a project by a group of executives of the Senior Management Programme studying at the Lagos Business School is making a difference
At the Maternal and Child Centre on Ogombo Road in Eti-Osa, Lagos, the consequences of power outage have been devastating.
Months ago, a newborn died in the hospital’s 38-bed Neonatal Intensive Care Unit when power suddenly failed, plunging the ward into darkness and bringing life-saving machines to an abrupt halt.
The silence that followed was fatal.
In another case, a fragile infant slipped into severe hypothermia after prolonged exposure when essential equipment stopped working during an outage.
For over 18 hours, doctors and nurses fought to stabilise the baby, pushing the limits of endurance and hope.
Chief Nursing Officer, Modupe Nasiru, was there when both incidents happened.
For her, they were not isolated incidents, but part of a troubling pattern.
“If babies are not kept in incubators and there is no constant power supply, due to the lack of sufficient subcutaneous tissue or fat, they may develop what we call hypothermia.
“Hypothermia can be fatal. Once their temperature drops, it becomes extremely difficult to bring it back up,” Nasiru explained.
Her voice carries the weight of experience.
In the NICU, there are no minor setbacks, only consequences.
Built to survive
The neonatal intensive care unit is designed to care for newborns aged zero to 28 days, the most vulnerable stage of human life.
Many of the babies admitted here are premature, underweight, or battling life-threatening complications.
Their survival depends not on instinct or strength, but on machines.
Incubators regulate body temperature. CPAP machines assist breathing. Phototherapy units treat jaundice.
Monitors track heart rate, oxygen saturation, and respiration. Infusion and syringe pumps deliver life-saving medications in precise doses.
Every one of these systems depends on electricity.
“When you walk into the NICU, you are not just seeing babies. You are seeing lives that are completely dependent on power,” Nasiru said.
Without it, the entire system collapses.
When lights go out
When Nasiru resumed at the hospital in December 2024, the power supply was relatively stable.
Outages occurred, but they were brief and manageable.
Medical teams could respond quickly, and critical care was rarely interrupted.
That stability did not last.
Road construction along the Ajah axis coincided with repeated disruptions to the hospital’s electricity supply.
Underground cables were suspected to have been damaged, triggering prolonged outages that stretched from hours into days.
“What followed was something we had never experienced at that level. There were times we went days without power,” Nasiru said.
The hospital relied heavily on its generator, but generators are not fail-safe.
They require fuel, maintenance, and careful management.
Even under ideal conditions, there are gaps in the moment between shutdown and restart.
In a neonatal unit, those moments are dangerous.
“There were times we needed to suction a baby immediately or respond to aspiration,” Nasiru said.
“Without power, everything becomes slower, more difficult, more risky.”
In those moments, healthcare workers are forced to improvise, often with limited success.
Most vulnerable victims
Power outages do not affect all patients equally. In the NICU, the smallest babies suffer the most.
Preterm infants, commonly referred to as “born too soon,” lack the body fat needed to regulate their temperature.
Without incubators or radiant warmers, they lose heat rapidly.
“When power goes out, their temperature drops very quickly and once it drops, it is extremely difficult to restore,” Nasiru explained.
The consequences can be fatal.
Respiratory distress presents another challenge.
Many newborns require assistance to breathe, provided through CPAP machines that rely on electricity.
“We have several machines, but without power, they cannot function. If multiple babies need support at the same time, it becomes a serious limitation,” she said.
Babies with neonatal jaundice face a different but equally dangerous threat.
Without phototherapy, bilirubin levels rise, increasing the risk of brain damage and death.
“When there is no power, instead of improving, the condition worsens. That can lead to more invasive treatments and longer hospital stays,” she added.
In every case, the absence of electricity transforms manageable conditions into life-threatening emergencies.
A system under strain
The impact of power outages extends beyond medical equipment; it disrupts the entire ecosystem of care.
Nurses are forced to ration oxygen. Doctors struggle to perform procedures in poor lighting.
Electronic medical records also become inaccessible, forcing staff to rely on manual documentation.
“At some point, we had to start covering the babies to retain warmth. We were doing everything possible just to keep them stable,” Nasiru said.
Even routine tasks become difficult.
“When a doctor wants to insert a line, and there is no light, visibility becomes a challenge. It affects everyone—nurses, doctors, engineers,” she added.
The stress is constant. The margin for error is thin. And the cost, too often, is human.
Living on diesel
To keep the NICU running, Sunday PUNCH gathered that the hospital depended heavily on a 400 kVA generator.
It runs for up to 20 to 24 hours daily, consuming large volumes of diesel.
The Medical Director of the hospital, Dr Olufemi Aletan, said the situation was unsustainable.
“In the last five months or thereabouts, we had what I can term an energy crisis. The hospital experienced a very poor power supply from Eko Electricity Distribution Company, and the last five months were critically bad to the extent that, for weeks, we did not even have electricity for one hour,” he stated.
The financial burden was immense.
Diesel prices had soared to N1,850/litre, eroding hospital resources and limiting its ability to invest in other critical areas.
“Even when you want to switch off the generator briefly, it poses a risk. Those babies cannot afford even a few minutes without power,” he said.
The hospital explored alternatives, including acquiring additional generators.
But each option came with the same challenge, fuel costs and long-term sustainability.
LBS: A ray of hope
As the hospital was considering other possible options, help came from an unexpected direction.
A group of executives from different organisations enrolled in the Senior Management Programme at the Lagos Business School identified the hospital’s energy challenges as an opportunity for impact.
Rather than providing temporary relief, they sought a lasting solution.
Their answer was solar energy.
Installed in March 2026, the solar system was designed to provide uninterrupted power to the neonatal unit.
It consists of 28 high-capacity solar panels, inverter systems, and lithium battery packs capable of storing and delivering energy round the clock.
According to the hospital’s Head of Engineering, Awolusi Oluwaseun, the system has transformed operations.
“It provides 24-hour electricity, depending on the load. It is reliable enough to support sensitive medical equipment,” he said.
Oluwaseun noted that the hospital’s engineering team would carry out regular maintenance to ensure the system continues to operate efficiently.
From darkness to stability
Since the installation, the difference has been profound.
“Before, whenever the generator failed, we would have a total blackout. Now, that no longer happens,” Nasiru said.
The constant fear of sudden outages has also eased.
Medical staff can focus on care rather than contingency plans. Equipment runs without interruption.
The impact is most visible in the babies themselves.
Nasiru recalled a particularly delicate case of a preterm infant weighing just 0.7 kilograms at admission.
“Such a baby cannot survive without constant power. This is why uninterrupted electricity is not optional in the NICU,” she said.
Globally, not much progress has been made in reducing neonatal mortality, especially in Africa.
Data from the United Nations Children’s Fund showed that approximately 2.3 million children died within their first month of life in 2024, which is equivalent to about 6,200 neonatal deaths each day.
The burden is disproportionately concentrated in developing regions.
In 2024, neonatal mortality rates were highest in Sub-Saharan Africa and South Asia, at 26.6 and 21.1 deaths per 1,000 live births, respectively.
A child born in Sub-Saharan Africa is more than 11 times more likely to die in the first month of life than a child born in Western Europe, while a child in South Asia faces a risk nine times higher.
According to the Global Economy, Somalia recorded Africa’s highest neonatal mortality rate in 2023 at 35 deaths per 1,000 live births, followed by Niger and Nigeria, both at 34 deaths per 1,000.
At the Maternal and Child Centre, Ogombo, hospital records reflect both the scale of demand and the fragility of outcomes.
In 2025, the neonatal unit recorded an average of 77 admissions per month, with a corresponding average of two deaths monthly.
The mortality figure, though modest at a glance, underscores a deeper reality: in neonatal care, even a single preventable death is one too many.
Experts attribute much of this to gaps in infrastructure, including unreliable electricity.
A paediatric cardiologist, Dr Oyinkansola Agaja, said a consistent power supply is critical.
“Electricity directly affects outcomes in neonatal care. Without it, even basic interventions become unsafe,” she said.
Agaja noted that while hospitals attempt to adapt, these adjustments are often inadequate.
“Modifications are never as effective as proper equipment functioning under stable power,” she added.
The executives
A representative of the LBS SMP 99 cohort, Group Two, Dr Michael Akpoarebe-Isaac, said the 18-member group was inspired to give back to society.
Akpoarebe-Isaac, who is also the Chief Executive Officer of Health Partners HMO Limited, noted that beyond government efforts, everyone has a role to play in developing their community and addressing critical gaps in maternal and child health.
He said, “By virtue of the training we have received at the Lagos Business School, because of our Senior Management Programme, we have been inspired to give back to society. We realise that beyond the government, everybody has a role to play in developing society, whether at the level of human capital or infrastructure.”
He explained that the neonatal unit of the hospital required urgent support, particularly the services it provides to neonates and the high-tech equipment essential for their survival, which depend on a reliable power supply to be effective.
Akpoarebe-Isaac pointed out that infrastructural gaps are a major contributor to Nigeria’s high maternal and child mortality rates.
“If you look at the statistics of maternal mortality or child mortality in Nigeria, we have one of the worst indices in the world. Infrastructural gaps are a major driver of these indices, and at a centre like the maternal and child centre, irregular power supply limits the medical team’s ability to provide the best care, especially for newborns in their first 20 days of life.
“Most babies in this public facility are from families that cannot afford private healthcare and among these children are future leaders and professionals. In our view, the least we can do is to give them the best fighting chance to ensure that they survive,” he said.
He also emphasised the role of the private sector in healthcare development, noting that public institutions are often overwhelmed and inadequately equipped.
Aside from Akpoarebe-Isaac, the group includes Asma’u Maibe of FGN Power Company; Franklin Amadi, Austin Akuma, and James Ezenwa of Keystone Bank; Princewill Alozie and Emazino Ewhero of Unilever Nigeria Plc; Ifeoma Adeyinka of Atreos Retail Platform; and Ediagbonya Osas of ARM Investment Managers.
Also on the team are Adetola Kolapo of NNPC Limited; Gloria Okereke of IHS Towers Limited; Osuji Ngozi and Adekola Alonge of Union Bank Plc; Eseoghene Oyibo of Blaaiz Innovations Technology Ltd; Morenike of NBC; Nafisa Rugga of the Nigerian Communications Commission; Yomi Arowosafe of the Universal Service Provision Fund; and Samson Folarin of PUNCH.
Together, they reflect a broad representation of finance, energy, telecommunications, media and technology professionals.
A manager at the LBS, Christiana Ogoko, explained that the institution organised members of the SMP 99 cohort into groups to implement life-changing projects that would positively impact their communities.
Ogoko said the SMP is designed for senior and mid-level managers who lead teams or business units and wish to enhance their effectiveness.
According to her, executives preparing to assume broader strategic or cross-functional roles, as well as professionals seeking to strengthen their leadership, analytical, and decision-making capabilities also participate in the programme.
Govt lauds initiative
The Lagos State Government, while reacting to the project, lauded the executives for supporting government efforts in the health sector.
The state Commissioner for Information and Strategy, Gbenga Omotosho, said the initiative was also a challenge to other corporate organisations.
He said, “The Mother and Child Centre is one of the new hospitals that the administration of Governor Babajide Sanwo-Olu built in his first tenure. I remember that there was a time he paid an unscheduled visit to the hospital and met many mothers and children at the hospital. He also asked for the number of deliveries at the hospital and they told him. They were very happy to see him.
“So, if corporate groups are doing this to support the government, it is very good. Because the government cannot do it alone, no matter how good and powerful a government may be, there will always be room for support like this.
“And when good citizens show love, compassion and character through initiatives that will ensure 24 hours power supply, it shows that our humanity is still intact. It is highly commendable.”
Where light means life
When Sunday PUNCH visited the hospital, the atmosphere had changed.
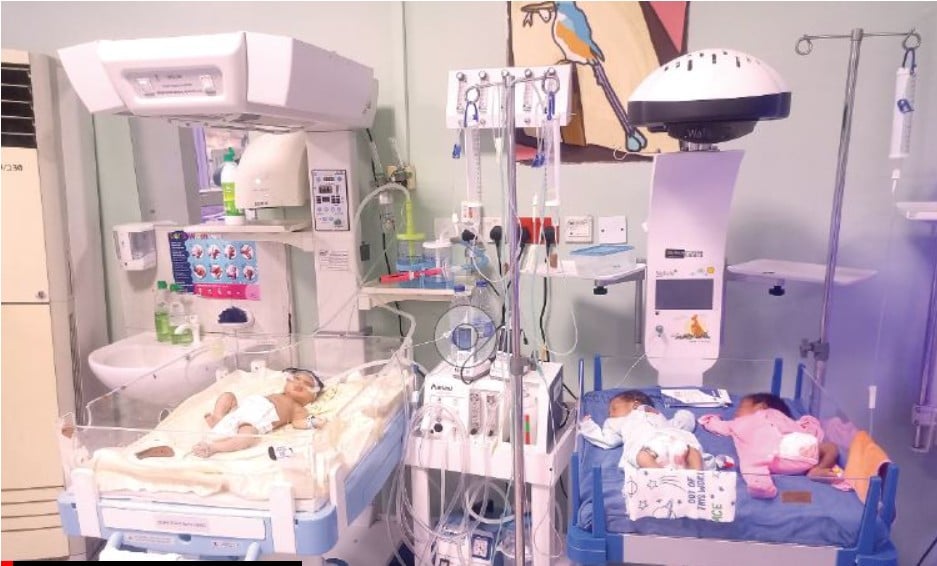
The constant hum of machines was steady and reassuring. Incubators glowed softly, maintaining the fragile balance between life and death.
Nurses moved with greater confidence.
The babies lay quietly, connected to tubes and monitors.
They still depended entirely on technology.
But now, that technology works when it is needed most.
The medical director, Dr Aleta, said the initiative is a breath of fresh air.
“It will not only save lives, but reduce the amount of diesel we consume, especially now that diesel prices are high and significantly impact the hospital’s finances. I must say I am grateful to the Lagos Business School for what they have done.
“In the neonatal unit, newborn babies are admitted, and anything that affects them impacts both their survival and their future potential. There is no doubt that both morbidity and potential mortality will be reduced by this intervention,” he added.
The MCC is now different.
When lights go out elsewhere, here, they stay on and that difference is the thin line between life and death.