By Punch Editorial Board
ON April 25, the global community marked World Malaria Day 2026 with an urgent theme, “Driven to End Malaria: Now We Can. Now We Must.” This message is a call to action anchored on a rare convergence of scientific progress and global resolve.
For Nigeria, where malaria remains a persistent public health burden, the message demands more than commemoration; it requires decisive, sustained action.
In a statement to mark the day, the WHO noted that, with rapid advances in science, “for the first time, ending malaria in our lifetime is a real possibility.” That assertion would have seemed far-fetched just a decade ago.
Today, however, it reflects tangible progress: new vaccines, improved treatments, next-generation mosquito control tools, and even pioneering technologies such as genetically modified mosquitoes and long-acting injectables are no longer theoretical; they are in various stages of development and deployment.
Encouragingly, 25 countries are already rolling out malaria vaccines, targeting about 10 million children annually.
Next-generation mosquito nets now account for 84 per cent of all new nets distributed globally, while nationally led programmes are increasingly shaping tailored responses to local realities. These are not abstract gains; they are measurable strides toward a long-elusive goal.
The numbers further illustrate this progress. According to the WHO, 37 countries reported fewer than 1,000 malaria cases in 2024, while 47 countries have been certified malaria-free.
Yet, even as progress is recorded, troubling signals remain. There were 610,000 malaria-related deaths globally, a slight increase from 2023, underscoring the fragility of recent gains.
Nigeria carries the world’s highest malaria burden. The country accounts for roughly 24 per cent to 27 per cent of global cases and 30 per cent to 31 per cent of global deaths, with over 68 million estimated cases and nearly 200,000 deaths annually. Malaria causes 30 per cent of hospital admissions, predominantly during the rainy season.
This levies a huge burden on the system. The Minister of Health, Ali Pate, said it set back the GDP $1.1 billion annually due to treatment cost, absenteeism and lost productivity. It compounds poverty due to the out-of-pocket spending, which is between 66 per cent and 76 per cent in Nigeria.
“In 2022, over 180,000 Nigerian children under the age of five lost their lives to malaria,” Pate lamented.
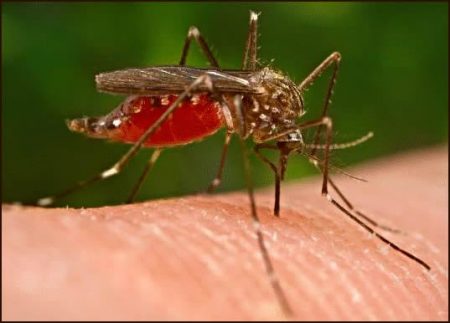
Malaria remains a complex disease, transmitted by the female Anopheles mosquito, which carries the parasite responsible for infection. Once bitten by an infectious mosquito, symptoms do not appear immediately.
The incubation period, typically between seven and 30 days, can vary depending on the species of parasite involved, according to the Africa Centre for Disease Control and Prevention. In some cases, symptoms may manifest as early as one week or as late as a year after infection.
When symptoms do emerge, they are often debilitating: fever, chills, headache, muscle aches, fatigue, nausea, vomiting, and diarrhoea. Without prompt and effective treatment, malaria, especially that caused by Plasmodium falciparum, the deadliest strain prevalent in Africa, can quickly become fatal.
For decades, the backbone of malaria treatment has been artemisinin-based combination therapy. Alongside this, the RTS,S/AS01 vaccine, the first to demonstrate partial protection against malaria in young children, represents a milestone in prevention.
Combined with vector control strategies such as insecticide-treated mosquito nets and indoor residual spraying, these interventions have saved millions of lives.
However, the optimism surrounding scientific progress is tempered by emerging biological threats that could undermine decades of hard-won gains. The World Malaria Report 2025 highlights several alarming trends.
First is drug resistance. Partial artemisinin resistance has now been confirmed in four African countries: Eritrea, Rwanda, Uganda, and the United Republic of Tanzania, and it is spreading.
This development poses a direct threat to the most effective treatment currently available.
Second is insecticide resistance. Resistance to pyrethroids, the primary chemicals used in bed nets, has been confirmed in 48 of 53 reporting countries, significantly reducing the effectiveness of one of the most widely deployed preventive tools.
Third is diagnostic failure. Gene deletions, specifically pfhrp2, are increasingly rendering rapid diagnostic tests unreliable. These deletions have now been reported in 46 endemic countries, complicating efforts to detect and treat malaria promptly.
Adding to these challenges is the emergence of invasive mosquito species. Anopheles stephensi, an urban-dwelling and insecticide-resistant mosquito, is expanding its footprint across Africa, posing a new and particularly dangerous threat to densely populated cities.
Beyond biological threats, systemic challenges threaten to derail global malaria control efforts. Chief among these is a severe funding crisis. In 2024, global funding for malaria stood at $3.9 billion, a figure less than half of the $9.3 billion target for 2025. This leaves a staggering shortfall of $5.4 billion, creating a dangerous gap between ambition and reality.
Reports by Health Policy Watch paint an even grimmer picture. The Global Fund’s eighth replenishment raised only $12.64 billion against a target of $18 billion, leaving a $5 billion deficit. Key donors are pulling back: France has slashed its contributions by 58 per cent, while the United States has also reduced its commitments.
As a result, the Global Fund is allocating $10.78 billion for the 2026–2028 cycle, the lowest level since 2020, representing a decline from previous funding rounds. The impact is already evident.
By early 2025, more than 40 per cent of planned insecticide-treated net distributions were either delayed or at risk.
The consequences of this funding crisis could be severe. Combined with climate change and rising resistance to insecticides, reduced funding raises the spectre of a major resurgence in malaria cases, potentially leading to hundreds of thousands of additional deaths by 2030.
Even the rollout of new vaccines, expected to be a game-changer in 2026, is under threat due to limited resources. Supply chains are also under strain, with several countries reporting critically low stocks of rapid diagnostic tests and essential medicines.
This is a stark reminder that scientific breakthroughs alone are insufficient. Without robust systems to deliver them, their impact will remain limited.
Sadly, Nigeria is not insulated from these challenges. The Federal Government currently spends $150 million annually on vaccine procurement, according to the Executive Director of the National Primary Health Care Development Agency, Muyi Aina.
These funds cover procurement, outbreak response, and logistics, including syringes, waste management systems, incinerators, and cold chain equipment.
However, this funding model relies significantly on support from development partners, particularly Gavi, the Vaccine Alliance.
As donor contributions decline, countries like Nigeria are increasingly expected to shoulder a larger share of the financial burden.
This shift underscores the urgent need for stronger domestic financing mechanisms.
On the prevention front, Nigeria has made notable progress. Since 2009, more than 320 million insecticide-treated nets have been distributed nationwide. Recent campaigns between 2025 and 2026 alone have delivered 3.1 million nets in Ogun State, 3.9 million in Akwa Ibom, and 4.4 million in Bauchi.
Yet, distribution does not always translate to utilisation. Many households report low usage rates, often citing discomfort caused by heat. This gap between access and use highlights the need for behavioural interventions alongside material distribution. Efforts to transition toward local manufacturing of mosquito nets may also help address supply challenges and reduce costs in the long term.
Ending malaria in Nigeria will require a multi-pronged approach anchored in sustained and diversified financing. High-impact, data-driven interventions must take precedence, ensuring that limited resources deliver maximum value.
Equally important is the need to channel more resources into the health sector, revive and rehabilitate decrepit primary healthcare centres, and ensure that interventions are tailored to specific community needs.
Nigeria needs research into simpler and cheaper but highly effective diagnostic tools. The universities should be tasked with this.
State governments should play a sterling role.
Interestingly, local solutions continue to play a role in malaria treatment. Ethnomedicine remains widely practised, with more than 60 indigenous plants used across Nigeria. While these traditional remedies are fraught with inconsistent dosing and a lack of scientific validation, some of these plants should be scientifically studied and standardised to identify active antimalarial compounds that could lead to the development of new drugs.
The tools to defeat malaria are within reach, but the commitment to deploy them at scale needs to improve. Nigeria needs to place more priority on health in national budgets, step up public awareness on malaria prevention and control, invest more in research and innovation to boost local vaccine production, and ensure that no community is left behind.
Copyright PUNCH
All rights reserved. This material, and other digital content on this website, may not be reproduced, published, broadcast, rewritten or redistributed in whole or in part without prior express written permission from PUNCH.