By Victor Ayeni
Although the term “myiasis” may not be widely familiar to many Nigerians, its clinical manifestations are often easily recognised across age groups.
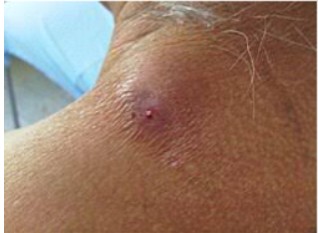
Myiasis is a parasitic infestation that affects both humans and animals, occurring either accidentally or as part of the parasite’s natural life cycle. It is caused by the larval stage of certain fly species and typically presents as large, painful, boil-like lesions that can develop on various parts of the body.
The term “myiasis” was first introduced in 1840 by an English entomologist, William Hope, who described the infestation of tissues and body cavities of living vertebrate hosts by the eggs or larval stages of dipteran flies.
According to a study published in the Ghana Medical Journal in 2020, the word is derived from the Greek “mya,” meaning fly, and “iasis,” meaning disease.
Ear, nose and throat specialists have also noted that different species of flies can induce myiasis in the head and neck region, with varying degrees of invasiveness and severity.
In 2021, The Nation reported cases among internally displaced persons, particularly women, who had fled insurgency and banditry in the North-East to the Federal Capital Territory. Many of them suffered from the condition.
One such case involved a 25-year-old pregnant mother of two who noticed what she described as a “huge boil” in her private area but delayed seeking help. It was only after her neighbour, Hajara Suleiman, visited to check on her that the severity of her condition became clear.
After raising the alarm, older women in the camp intervened.
“We cleaned the affected part with hot water and salt, then pressed it for the maggot to come out. Her screams filled the camp because the pain was worse than childbirth. When it finally came out, it was the largest I had ever seen,” Suleiman recounted.
Mothers’ nightmare
Although myiasis affects people of all ages and genders, it appears to be more common among children and is often first noticed by their mothers.
Recounting her son’s ordeal, Mrs Christiana Ibiam, a mother of two, said she was alarmed when she discovered two reddish, painful boils on his back.
“He was in pain and couldn’t go to school for days. He later developed a fever, so I called my mother. She came and applied palm oil on the boils.
“To my surprise, two maggots wriggled out. I had never seen anything like that. I later learnt that flies had laid eggs on his clothes, and the larvae burrowed into his skin,” she told Sunday PUNCH.
Similarly, a Lagos-based teacher, Sade Lamina, recalled her first encounter with myiasis through a nine-year-old pupil.
“She complained of discomfort and showed me boils on her arm. At first, we thought they were ordinary boils, but the school matron identified it as myiasis. We applied Vaseline, and a maggot was extracted.
“She had worn clothes that were dried on grass and not ironed. Flies had laid eggs on them,” Lamina explained.
In another case shared on Facebook, Mbah Chinwe recounted how what appeared to be harmless rashes on her baby’s back quickly escalated into something far more serious.
Initially dismissed and treated with over-the-counter cream, the rashes worsened, swelling into hardened lumps. Even antibiotics purchased later did not help. The baby became restless, irritable, and unable to sleep.
Then came the shocking discovery.
“I saw something white, like pus, on one of the boils. I tried to clean it, but it didn’t move. When I pinched it slightly, it came out; it was a maggot,” she said.
Further checks revealed more larvae beneath the skin, prompting an urgent hospital visit. Eventually, six maggots were extracted after applying thick palm oil to draw them out.
Cycle of infestation
Experts explain that certain flies common in tropical regions lay eggs on damp clothes left to dry outdoors.
When such clothes are worn, the larvae hatch due to body heat and burrow into the skin, leading to painful lesions.
According to the Centres for Disease Control, several genera of flies can cause myiasis in humans, including Dermatobia hominis (human bot fly), Cochliomyia hominovorax (New World screwworm), Chrysomya bezziana (Old World screwworm), and Cordylobia anthropophaga (tumbu fly).
The larvae typically develop beneath the skin, feeding in a subdermal cavity for weeks before emerging to continue their life cycle.
Recognising the signs
A registered nurse, Ruth Ita, explained that myiasis often presents with persistent itching or a crawling sensation under the skin, small, moving lumps or sores that do not heal, foul-smelling discharge, redness, swelling, or irritation, low-grade fever or general discomfort
A Senior Medical Registrar, Dr Paul Anejodo, added that the condition exists in different forms, including nasal, migratory, intestinal, and furuncular myiasis, the latter being the most common and resembling boils.
He warned that complications can be severe, particularly in areas with limited access to healthcare.
Tackling myiasis
Medical guidance suggests that treatment may involve suffocating the larva (occlusion), irrigation, manual extraction, or surgical removal in complex cases.
A medical laboratory scientist, Dr Ernest Ohanu, noted that the condition is more prevalent in humid regions such as the Niger Delta and peaks during the rainy season.
He explained that myiasis is often misdiagnosed as bacterial boils, leading to ineffective antibiotic use.
Myiasis is often mistaken for common bacterial boils (furunculosis) or cellulitis, leading to unnecessary antibiotic use. However, clues to look for include the ‘punctum’—a small hole at the centre of the boil used by the larva for breathing, a distinct ‘crawling’ or ‘tugging’ sensation under the skin, serosanguinous (bloody or watery) fluid leaking from the hole, and failure of antibiotics. If a boil does not respond to standard antibiotics, myiasis is a likely suspect,” Ohanu explained.
He noted that although all age groups are affected, infants and children are most vulnerable due to their tender skin and frequent contact with laundry or soil.
“It is highly endemic in the Niger Delta (Rivers, Bayelsa, etc.) and the South-East (Anambra, Enugu) due to the humid climate. Its treatment involves removing the larva from the skin. Occlusion therapy can also be used. This involves smothering the breathing hole with petroleum jelly (Vaseline), heavy oils, or adhesive tape. This suffocates the larva, forcing it to come to the surface for air, making it easier to pull out with forceps.
“Manual extraction can also be done. Once the larva is visible or partially emerged, it is gently extracted. It is vital not to crush the larva inside, as this can cause a severe allergic reaction or secondary infection. In complex cases (e.g., infestation in the eye or deep wounds), surgical removal by a healthcare professional is necessary,” Ohanu added.
Ohanu emphasised that prevention remains critical.
“Always iron clothes before wearing them, as heat kills any eggs or larvae. Avoid drying clothes directly on grass or shrubs. Maintain proper hygiene and environmental sanitation to reduce exposure to flies,” he advised.
Copyright PUNCH
All rights reserved. This material, and other digital content on this website, may not be reproduced, published, broadcast, rewritten, or redistributed in whole or in part without prior express written permission from PUNCH.