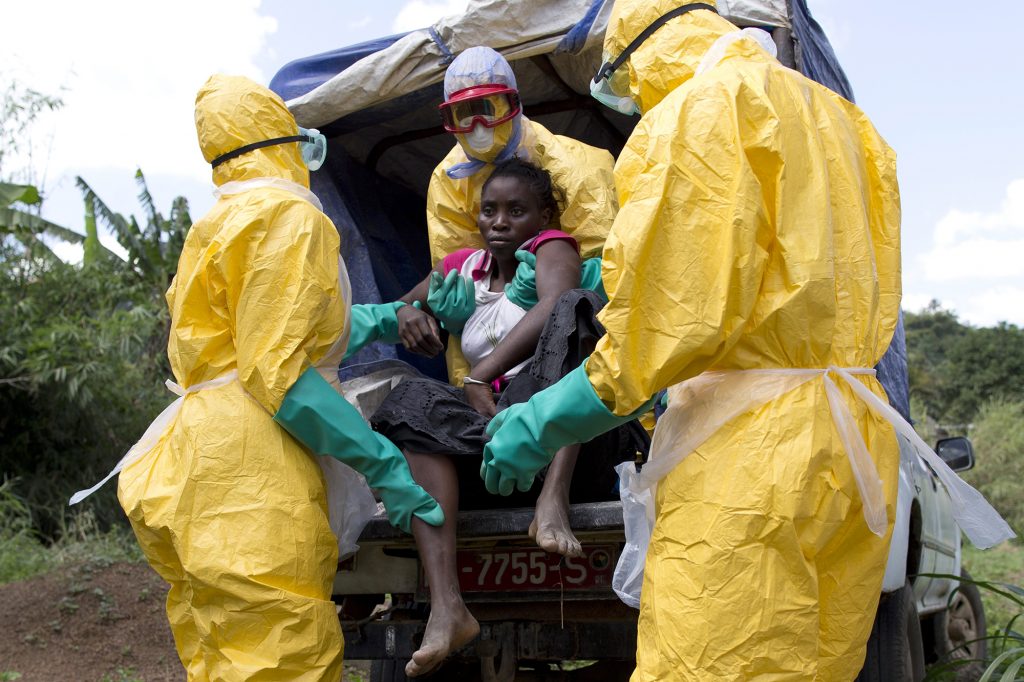
Experts have emphasised the critical role of trained personnel, reliable resources, and coordinated emergency systems in controlling epidemic outbreaks such as Ebola and COVID-19 during a high-level health security dialogue in Abuja.
At the session titled “Detection to Action: Emergency Response Systems and Coordination,” the Incident Manager, Polio Emergency Operations Centre, Dr Idowu Audu, said rapid deployment was central to containing outbreaks effectively and saving lives in crises.
Audu cited Nigeria’s experience during the Ebola outbreak in Lagos and early COVID-19 detection, where emergency response teams were deployed to affected areas within 24 hours, demonstrating the value of readiness.
He outlined three pillars of successful response: trained personnel, reliable operational resources, and robust digital and organisational systems tailored to the magnitude and complexity of each public health crisis.
“You don’t wait for presidential approval to act. Support and coordination are essential, whether from government, the private sector, or partners,” Audu said, highlighting the need for immediate, proactive measures.
He also emphasised accountability and clear role definition: “Everyone in the task force knows their responsibilities; outputs are documented, and alignment with state planning ensures a coordinated strategy,” he said.
Representatives from China’s Junshi Biosciences, including Mr Siyuan Wang, highlighted cross-border collaboration and innovation, explaining China’s integrated approach from drug development to global clinical trials and large-scale production during COVID-19.
Wang said that vaccines and biological drugs required ultra-cold storage and precise last-mile delivery: “The cloud-chain infrastructure allows storage and delivery from central hubs to local communities efficiently.”
From Nigeria, Senior Public Health Advisor, Ms Piring’ar Mercy Niyang, highlighted health system challenges, noting gaps in personnel, retention, and infrastructure in spite of more than 3,000 public health doctors for more than 200 million people.
She suggested leveraging community pharmacies and regulated pharmaceutical outlets for disease surveillance, monitoring, and rapid response, citing ATBTH Bauchi isolation centre as a model integrating local engineers and architects.
“Public health professionals cannot dictate urban planning or sanitation designs alone,” she said.
She emphasised the need to domesticate knowledge and integrate public health training into local curricula to grow national capacity.
The WHO Health Cluster Coordinator, Dr Aurelien Pekezou, highlighted the critical role of logistics in outbreak response, stressing that medicine production, distribution, and operational efficiency determined the effectiveness of vaccines in saving lives.
The AFENET Regional Coordinator, Dr Patrick Nguku, called for strategic planning, strong surveillance, efficient logistics, and adequate funding, referring to increased allocations as “vitamin M” essential for epidemic preparedness.
The News Agency of Nigeria reports that stakeholders ended building strong public health infrastructure, proactive planning, and international collaboration are vital for epidemic preparedness and resilient health systems in Nigeria and beyond.
They emphasised multi-level capacity building, from rural communities to urban centres, and coordination between public and private sectors as key to ensuring a timely response and national health security.
(NAN)